Table of Contents
What is Eczema?
Eczema is an uncomfortable and sometimes painful condition that affects over 31 million people in the United States. [1] Eczema, also known as atopic dermatitis, is an umbrella term used to describe several skin conditions. The types include atopic dermatitis, contact dermatitis, neurodermatitis, dyshidrotic eczema, nummular eczema, seborrheic dermatitis, and stasis dermatitis. All of these conditions cause dry, discolored, itchy, and inflamed skin. Eczema can affect people of all gender, age, or skin color.
Eczema is not only an uncomfortable physical condition but can affect a person’s mental health as well. The unsightly red bumps can make people feel self-conscious, which can worsen eczema. To maintain eczema, doctors may recommend several treatment options, including Neoral (cyclosporine) or Elidel Cream. Read on to learn more about the signs and symptoms of eczema. [1]
Eczema can be a chronic condition that flares up throughout a person’s life. It is more common in children, and some may grow out of it as they become older. For others, flare-ups may only occur every few years. Because this condition can occur at any age, it may present itself differently depending on the age of the person affected. Symptoms in children: A scaly and dry rash in the bends of the elbows, behind the knees, the neck, wrists, or ankles. [2] Symptoms in infants: An itchy rash that leads to oozing and crusting on the face and scalp. It may also occur on the arms, legs, back, and chest Symptoms of eczema in adults: A dry scaly rash on the face, back of hands, backs of knees, wrists, hands, or feet. In fairer skinned people, the skin may become reddish and turn brown. In darker-skinned people, the skin may become lighter or darker. [2] Additional symptoms can include: Several factors may lead to eczema flare-ups. Eczema can occur for several different reasons, and your doctor will help you figure out the cause. Common causes of eczema can include: This type of skin condition can run in families and is more common in those susceptible to allergies such as asthma and hay fever. If you have eczema, you also may be more prone to cold sores, warts, and athlete’s foot. [3] It is essential to seek diagnosis and treatment for eczema because the complications can be painful. Skin infections can become common because of repeated scratching that breaks and cracks the skin. You can tell if an infection is present if your eczema sores have red streaks, pus, or yellow scabs. Open skin can invite viruses into the body, like herpes simplex. If you have eczema for a long time, you can also develop chronic itchy skin. This condition is called neurodermatitis and results from scratching the same area, which makes it even itchier. Over time, you may begin to scratch this area out of habit even if it is no longer itchy. Irritant hand dermatitis can occur for those who work with their hands. It is most common in those who are constantly exposed to detergents, harsh soaps, and disinfectants. Along with all these maladies, sleep problems are also common. The itching and scratching cycle can lead to poor sleep quality. [4] Some people may not realize their eczema is serious until symptoms start to interfere with daily life. Many people will try home remedies at first, but if those do not work, you need to seek a doctor's help. Lab tests are not necessary for diagnosing eczema, so your doctor will diagnose you by examining your skin and asking about your medical history. If the doctor is unsure, they may implement patch testing to rule out other skin diseases. [4] There is no cure-all for eczema patients. This condition varies greatly, so you may have to try several treatment methods before finding one that works for you. In general, creams and oral medications are prescribed along with other home techniques. Creams: There are several different over-the-counter and prescription creams available to help with symptoms of eczema. Elidel Cream is a calcineurin inhibitor that is applied directly to the skin. It is an immunosuppressant that works by decreasing your body’s immune system to slow the growth of eczema on the skin. Other creams include corticosteroid creams, which can ease redness and reduce inflammation in the affected areas. [5] It is important to know the side effects of eczema creams because some can cause skin thinning if overused. It is essential to avoid strong sunlight when using these cream medications. [4] Antibiotics: Skin infections are fairly common in the case of eczema. Open and cracked skin is more susceptible to infections, so you may need antibiotic cream to fight bacterial infections. You may take oral or cream antibiotics to improve any skin infections. Oral Drugs: Several oral drugs can help control inflammation. Oral corticosteroids are used when the body does not respond well to other treatment methods. Neoral (cyclosporine) can be prescribed for severe cases of adult atopic dermatitis. It works by suppressing the immune system and blocks the body’s inflammation process. [6] Wet Dressing Therapy: Along with medications, you can also wrap the affected area. This is typically done in the hospital and involves wrapping the affected area with topical corticosteroids and wet bandages. This technique is only done for those with widespread lesions and requires nursing expertise. Your doctor and nurse can also help teach you how to do this at home. Light therapy: Light therapy is typically a last resort for those who do not respond well to other treatment methods. Light therapy (phototherapy) involves exposing the skin to controlled amounts of natural sunlight. This can also be done artificially, which involves using artificial UVA (ultraviolet A) and UVB (ultraviolet B) light. This can suppress overactive skin cells that cause inflammation. [4] The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis or treatment.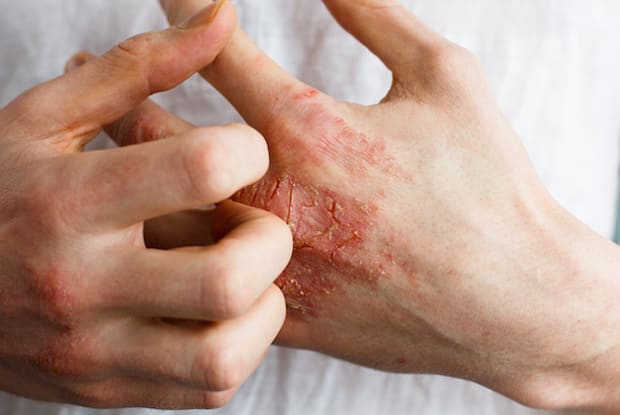
Symptoms of Eczema

What Causes Eczema?
Diagnosis
Treatment Methods