Table of Contents
I. Ulcerative Colitis Medications
II. Is Hospitalization Needed?
Ulcerative Colitis Medications
Ulcerative colitis (UC) is a chronic type of inflammatory bowel disease (IBD) that affects the gastrointestinal tract. This condition usually starts in the rectum and spreads upward, eventually affecting the entire colon. UC can cause the bowels to empty frequently. Additionally, ulcers can form on the surface of the bowels, causing bleeding and discharge.
Symptoms of UC can be very uncomfortable and disruptive. UC symptoms may include abdominal pain, bloody stools, rectal pain, weight loss, and diarrhea. Other parts of the body may also be affected by UC, and you may experience joint pain, skin problems, eye inflammation, and mouth sores. Most researchers think UC is the result of an overactive immune system, but genes, environmental factors, and other immune disorders may play a role.
If you are diagnosed with ulcerative colitis, the standard first line of treatment is with medications. Your doctor may use a stool test, endoscopy, colonoscopy, biopsy, or CT scan to confirm the diagnosis and rule out any conditions with similar symptoms. Mild symptoms are commonly treated with anti-inflammatory medications like Lialda (mesalamine) or Asacol (mesalamine) to reduce swelling. For moderate to severe UC symptoms, corticosteroids like Medrol (methylprednisolone) may be necessary. Corticosteroids are prescribed less often than anti-inflammatories because they can have adverse effects if overused. For certain cases of UC, your doctor may decide that biologics or immunomodulatory drugs are more suitable. [1] Those who have UC only require hospitalization if there are severe symptoms present. You should seek help from a doctor if you experience signs of liver disease, severe cramping, or dehydration. UC can lead to diarrhea, and diarrhea can cause serious loss of electrolytes, so you may need to visit a hospital if your electrolyte levels are low. If you lose too much blood from bleeding ulcers and blood in the stool, you may also need to seek a medical professional’s help to replace blood and treat any health complications that may occur. [2] Severe ulcerative colitis can lead to extreme blood loss from perforation of the colon. Serious blockages may also occur. In these instances, surgery may be required to remove the colon and create a new pathway for waste in its place. This pathway is typically placed through a small opening in your abdominal wall or connected back through the end of the rectum. If this surgery is successful, you will be able to pass stool through your rectum, but bowel movements will be more frequent than usual. [1] Because medical treatments for ulcerative colitis may cause serious side effects, many people opt to use natural remedies if they don’t react well to their UC drugs. Some types of natural treatments may be used in conjunction with prescription UC drugs, but you should always consult your doctor before adding new substances to your treatment plan to avoid adverse drug interactions. Below is a list of some common natural remedies for UC. Foods that are rich in fat content have a higher chance of causing diarrhea and UC flare-ups, so eating a low-fat diet may help bolster your treatment plan. Studies show that by eating low-fat foods, you can delay UC flares. Fats can be hard to avoid for many people. A good place to start is to replace your normal sources of fat with healthier options like olive oil, fish oil (omega-3 fatty acids), and avocados. As mentioned above, ulcerative colitis is thought to be caused by something wrong with the immune system. Upping your intake of vitamin C can help with UC symptoms by strengthening your immune system so you can recover faster after a flare-up. Parsley, bell peppers, spinach, and berries are great sources of vitamin C for UC patients and can help prolong periods of UC remission. Finally, increasing fiber intake during remission can help regulate bowel movements. However, be careful with fiber because eating fiber during a flare-up can contribute to your symptoms. [1] A UC-friendly diet is usually the first thing suggested by doctors if your UC is relatively new or mild. For more serious cases of UC, a healthy diet may need to be paired with the right medication for the best results. Ask your doctor about Asacol (mesalamine), Lialda (mesalamine), or Medrol (methylprednisolone) today. The only known cure right now is the removal of the entire colon and rectum, but you may still be able to manage your UC symptoms non-surgically with the right treatment plan. The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis, or treatment.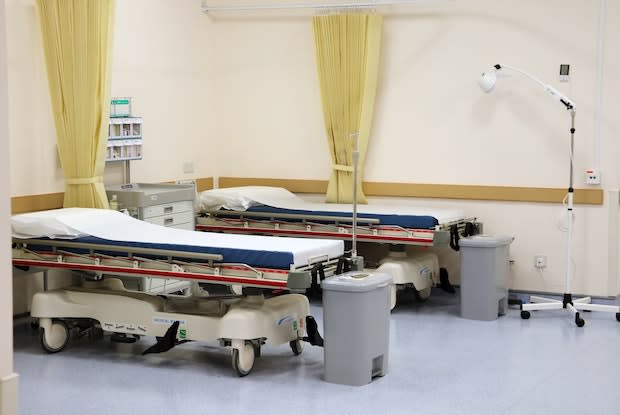
Is Hospitalization Needed?
Surgery for UC
Natural Treatment Options

UC-Friendly Diet

